CMS Publishes NGHP User Guide Version 6.9

by F. Fairchok
CMS published an update to the NGHP User Guide on October 3, 2022. Version 6.9 announced changes to the areas of ICD coding and SP31 error code usage.
Update Summary
In a major change regarding how CMS provides data relating to which ICD codes are valid (or not) to use for Section 111 reporting, the following changes have been made:
-
- CMS is providing ICD-10 and ICD-9 code lists via downloadable Microsoft Excel files that provide valid codes and define which codes are excluded by plan type. These files are located at: https://www.cms.gov/medicare/coordination-benefits-recovery-overview/icd-code-lists
- Appendix I is now titled “Excluded and No-Fault Excluded Diagnosis Codes” and provides general guidance to assist with understanding ICD code usage and exclusions. Previously, this appendix was titled “Excluded ICD-10 and ICD-9 Diagnosis Codes” and contained thirteen pages of excluded codes that have been removed and can now be found in the Excel files provided.
- Appendix J now contains information about “HEW Installation and Configuration”, where previously it contained a forty-page listing of “No-Fault Excluded Diagnosis Codes.”
- In addition to these structural changes to the User Guide’s Chapter V: Appendices, CMS also has updated the ICD code sets for reporting claims in 2023.
The second change announced in this User Guide update is that the SP31 error code has been restored. The summary of updates states “RREs will receive this error code when submitting records with effective dates greater than 90 days prior to Medicare entitlement (Appendix F).”
Commentary
In the November 10, 2020 update, NGHP User Guide version 6.1, CMS announced they were retiring the SP31 error code. In that update, CMS stated the following:
“Claim Input File Detail Records, and Direct Data Entry (DDE) records, submitted prior to the effective date of the injured party’s entitlement to Medicare will be rejected and returned with a Disposition Code ‘03’ instead of an SP31 error.”
With the current update, CMS is reinstating the SP31 error code, which will arrive with the SP disposition code that rejects the claim and forces the RRE (or reporting agent) to queue the record for resubmission in the following quarter. Back in 2020, some in the industry speculated whether the attempt to remove the rejection of the claim with the SP31 error was positioning by CMS to only produce error rejections on valid issues requiring correction by the RRE. We will need to see how this plays out as we await further movement of the Civil Money Penalties rulemaking and whether or not CMS makes additional changes to track the metric around error thresholds.
A final note, while drafting of this article we noted that the update was to NGHP User Guide version 6.9. However, the last published version we found was 6.7 from January 10, 2022. IMPAXX closely monitors changes to these guides through multiple means, therefore we do not believe version 6.8 was ever released publicly.
However, in the summary of changes for version 6.9 (Appendix M, page 214) there is a reference made to a version 6.8 as follows:
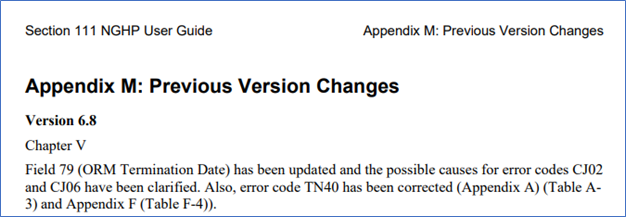
Figure 1 – NGHP User Guide 6.9, Chapter V, page 214
To provide a thorough analysis, we compared version 6.7 to 6.9 and documented the following changes:
-
- Text has been added to the ORM Termination field description text that states:
“If no ORM Termination Date is provided but an Exhaust Date for Dollar Limit for No-Fault Insurance (Field 62) is provided, then this date will be used to auto populate the ORM Termination Date.”
-
- The “Possible Cause” text for error code TN40 has been corrected to state:
Field 24: is “Y” and there is not an established active MSPRP account for a recovery agent TIN submitted in (field 25)
In version 6.7 the field attributed to this error was field 25.
-
- Minor clarifications have been added around the use of error codes CJ02 and CJ06 when submitting ORM Termination Dates.
The links to the NGHP User Guide, version 6.9 can be found here.
If you have questions regarding this article and/or any changes made in version 6.9 of the user guide, please don’t hesitate to email us at [email protected]. If you are looking for further guidance on Section 111 reporting compliance, our experienced Medicare Secondary Payer Reporting services team collaborates with clients to customize their compliance experience and meet their unique needs and requirements. Contact us today to learn more.